The Deadly Cancer Hiding in Plain Sight and Why Most Patients Never Get Screened
NEWNow you can listen to News articles!
A new study from Northwestern Medicine suggests that current lung cancer screening guidelines may be missing the majority of Americans who develop the disease, and researchers say it’s time for a major change.
Published in JAMA Network Open, the study looked at nearly 1,000 lung cancer patients who were treated at Northwestern Medicine between 2018 and 2023.
The goal was to see how many of those patients would have qualified for screening based on existing U.S. Preventive Services Task Force (USPSTF) guidelines.
HIDDEN BREAST CANCER THAT IS HIDDEN FROM EXAMS ORIENTED IN INNOVATIVE TECHNOLOGY
Currently, the USPSTF recommends annual CT scans for adults ages 50 to 80 who have a smoking history of 20 pack years (the equivalent of one pack of cigarettes per day for 20 years). and still smoke or quit within the last 15 years.
Only about 35% of those diagnosed with lung cancer met the current criteria for screening.
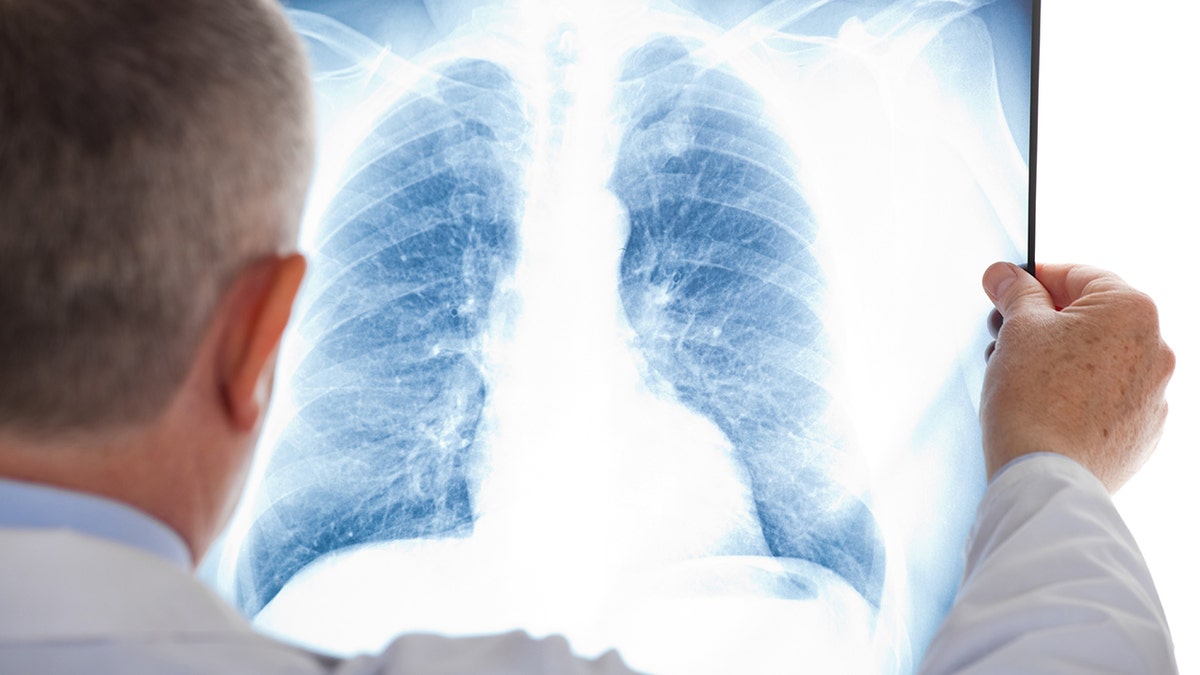
Current lung cancer screening guidelines may be missing the majority of people who develop the disease, a new study shows. (iStock)
That means about two-thirds of patients would not have been selected for testing before their diagnosis.
“That approach not only misses many patients who had quit smoking in the past or who did not meet high-risk criteria, but it also misses other patients at risk for lung cancer, such as non-smokers,” Dr. Luis Herrera, a thoracic surgeon at Orlando Health, told News Digital.
The study noted that these patients tended to have adenocarcinoma, the most common type of lung cancer among never smokers.
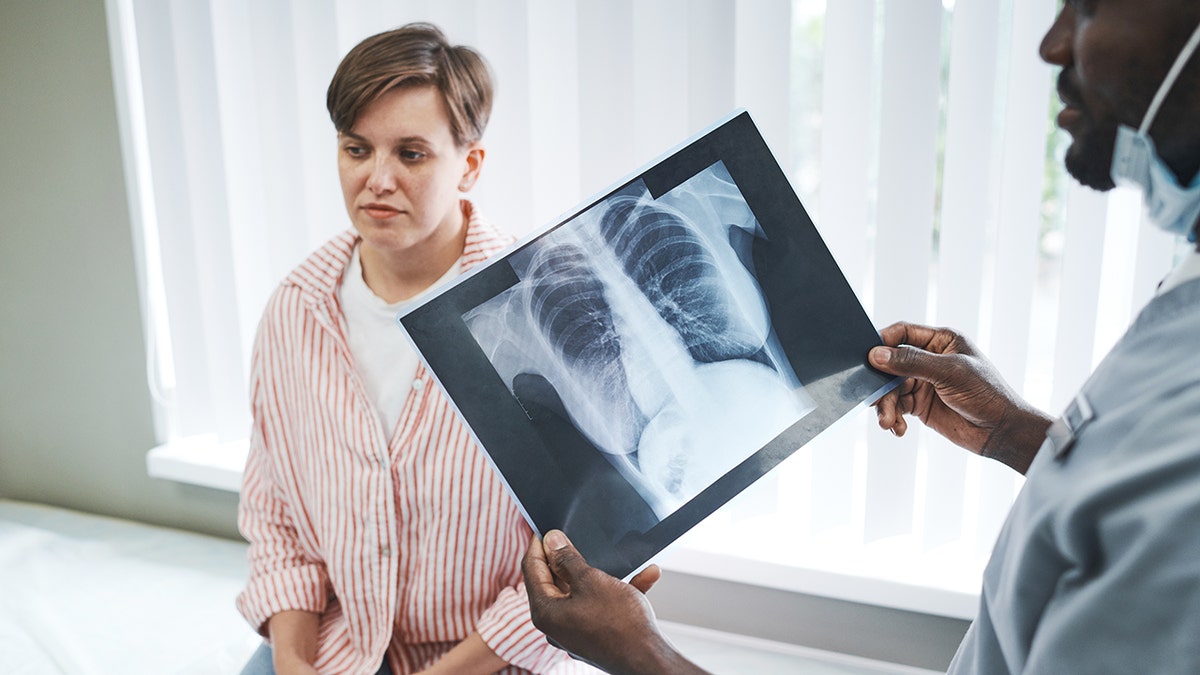
The ignored patients tended to have adenocarcinoma, the most common type of lung cancer among never smokers. (iStock)
Those not meeting the guidelines were most often women, people of Asian descent and people who had never smoked, the study found.
The research team also compared survival outcomes. Patients who did not meet screening criteria had better survival, living a median of 9.5 years compared with 4.4 years for those who did qualify.
ERIN ANDREWS ‘DID NOT HAVE SYMPTOMS’ BEFORE CANCER DIAGNOSIS, PURSUE FOR EARLY SCREENINGS
While this difference partly reflects tumor biology and earlier detection, it also highlights how current screening rules fail to detect a wide range of cases that could be treated earlier, according to the researchers.
“Current participation in lung cancer screening for patients who qualify based on smoking history is quite low,” said Herrera, who was not involved in the study. This is likely due to the complexity of the risk-based criteria and the stigma associated with smoking and lung cancer, he added.
CLICK HERE FOR MORE HEALTH STORIES
To test an alternative, the researchers modeled a different approach: testing all people between 40 and 85 years old, regardless of their smoking history.
Under that universal age-based model, about 94% of the cancers in their cohort would have been detected.
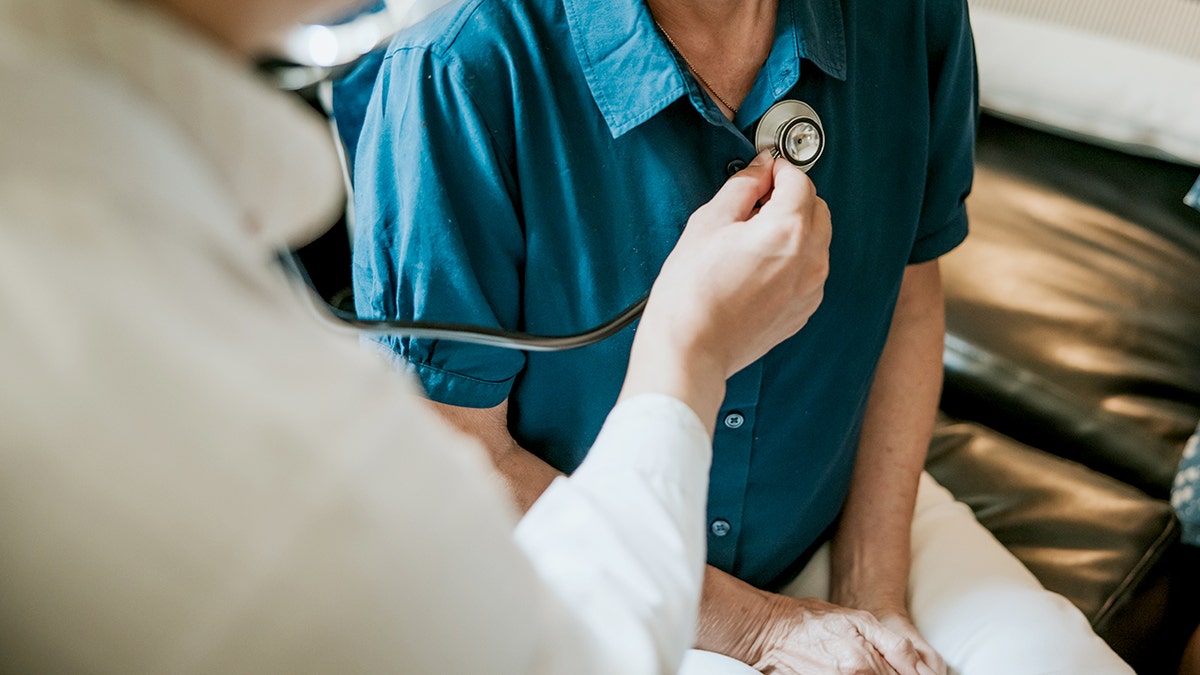
Universal screening procedures could save lives and hundreds of thousands of dollars, researchers say. (iStock)
Such a change could prevent approximately 26,000 deaths in the United States each year, at a cost of about $101,000 per life saved, according to their estimates.
The study emphasized that this would be much more cost-effective than current breast or colorectal cancer screening programs, which cost between $890,000 and $920,000 per life saved.
CLICK HERE TO SUBSCRIBE TO OUR HEALTH NEWSLETTER
Herrera highlighted the many challenges in lung cancer screening adoption, from lack of awareness to some providers not recommending screening.
However, he added, “the cost of screening tests is covered by most health insurance plans, and many institutions also offer discounts for patients who do not have insurance.”
“Current participation in lung cancer screening for patients who qualify based on smoking history is quite low.”
Lung cancer remains the deadliest cancer in the country, killing more people each year than colon, prostate and breast cancer combined. But because of narrow eligibility criteria based on smoking history, millions of at-risk people never get tested.
Northwestern Medicine researchers argue that expanding screening to include all adults within an age range could help close those gaps, especially for often underdiagnosed groups.

Researchers say expanding screening to include all adults could help detect missing cases. (iStock)
The study was conducted at a single academic center, meaning the patient population may not represent the general US population. It also analyzed existing data, so it cannot test how the new model would work in real-world screening programs, the researchers acknowledged.
CLICK HERE TO DOWNLOAD THE News APP
Cost and mortality projections are based on assumptions that could change depending on how screening is implemented.
The researchers also did not fully take into account the potential disadvantages of a broader evaluation, such as false positives or unnecessary follow-ups, they noted.
TRY OUR LATEST LIFESTYLE QUIZ
For patients who do not qualify for lung cancer screening, there are other opportunities for lung evaluations, including “cardiac calcium scores, CT scans, and other imaging modalities that can at least evaluate the lungs for suspicious nodules,” Herrera added.
Khloe Quill is a lifestyle production assistant at News Digital. She and the lifestyle team cover a range of topics including food and drink, travel and health.



