Cancer survival appears to double with common vaccine, researchers say
NEWNow you can listen to News articles!
A common vaccine could help fight cancer, a new study suggests.
For cancer patients undergoing immunotherapy, researchers found that receiving the COVID-19 mRNA vaccine within 100 days of starting immune checkpoint therapy was associated with substantially better survival.
Researchers from the University of Florida and the University of Texas MD Anderson Cancer Center analyzed data from more than 1,000 patients with stage 3 and 4 non-small cell lung cancer and metastatic melanoma who were treated at MD Anderson from 2019 to 2023.
5 THINGS YOU SHOULD KNOW BEFORE GETTING THE FLU SHOT, ACCORDING TO DOCTORS
All patients were treated with immune checkpoint inhibitors, a type of immunotherapy drug that helps the immune system recognize and attack tumor cells more effectively.
Some of the patients received an mRNA COVID vaccine within 100 days of starting immunotherapy and others did not, according to a news release from the study.

A common vaccine could help fight cancer, a new study suggests. (iStock)
The researchers found that those who received both the vaccine and immunotherapy lived longer “by a significant amount.”
Those who received the vaccine had almost double the average survival: 37.3 months compared to 20.6 months.
VACCINE DEBATE HEATS UP AS OFFICIALS ARE SPLITTING COMBINED MMR INTO SINGLE DOSES
The greatest survival benefit was seen in patients with immunologically “cold” tumors, those that are typically resistant to immunotherapy. Among those patients, the addition of the COVID-19 mRNA vaccine was associated with a nearly five-fold increase in three-year overall survival.
“At the time the data was collected, some patients were still alive, which means that the effect of the vaccine could be even stronger,” the statement states.
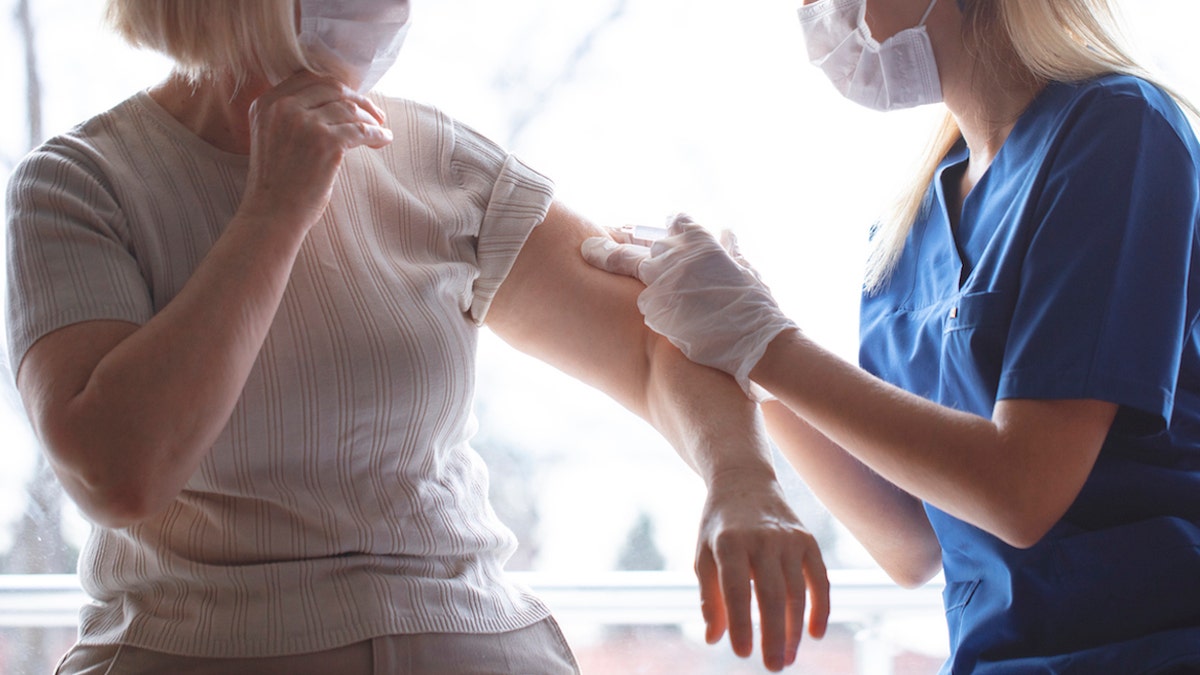
Researchers found that receiving the COVID-19 mRNA vaccine within about 100 days of starting immune checkpoint therapy was associated with substantially better survival. (iStock)
The researchers then replicated this result in mouse models: When the mice received a combination of immunotherapy drugs and an mRNA vaccine targeting the COVID-19 spike protein, their tumors responded better to the treatment.
“This is the type of treatment benefit that we strive for and hope to see with therapeutic interventions.”
The study found that non-mRNA vaccines for flu and pneumonia did not have the same effects.
The findings were presented at the European Society for Medical Oncology (ESMO) 2025 Congress in Berlin on October 19 and published in the journal Nature.
CLICK HERE TO GET THE News APP
“The implications are extraordinary – this could revolutionize the entire field of cancer care,” said principal investigator Elias Sayour, M.D., Ph.D., a UF Health pediatric oncologist and the Stop Children’s Cancer/Bonnie R. Freeman Research Professor in Pediatric Oncology.
As this was an observational study, the researchers noted that a prospective, randomized clinical trial is needed to confirm the findings.
CLICK HERE TO SUBSCRIBE TO OUR HEALTH NEWSLETTER
“Although it has not yet been proven causal, this is the type of treatment benefit that we strive for and hope to see with therapeutic interventions, but rarely do,” said Duane Mitchell, M.D., Ph.D., director of the UF Clinical and Translational Sciences Institute.
“I think the urgency and importance of doing the confirmation work cannot be underestimated.”
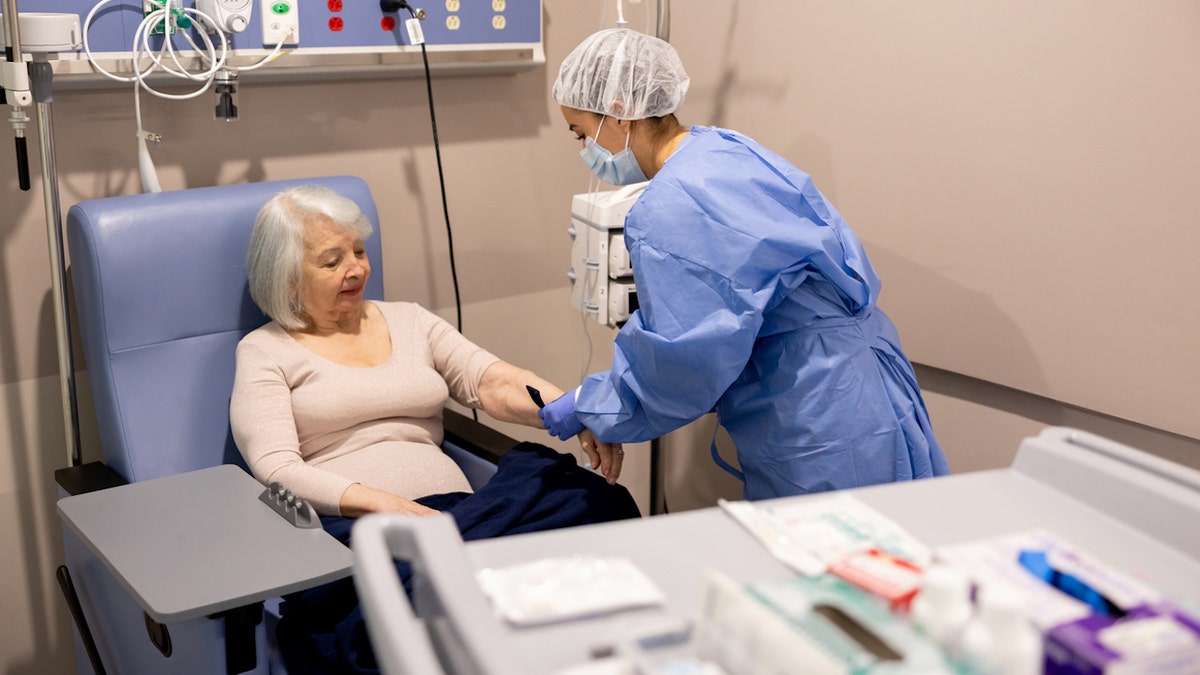
All patients were treated with immune checkpoint inhibitors, a type of immunotherapy drug that helps the immune system recognize and attack tumor cells more effectively. (iStock)
Researchers now plan to launch a large clinical trial through the UF-led OneFlorida+ Clinical Research Network, a consortium of hospitals, health centers and clinics in Florida, Alabama, Georgia, Arkansas, California and Minnesota, according to the release.
In the future, the researchers suggested that a “universal, ready-to-use” vaccine could be developed to boost the immune response and survival of cancer patients.
TRY OUR LATEST LIFESTYLE QUIZ
“If this can double what we’re currently achieving, or even incrementally (5%, 10%), it means a lot to those patients, especially if this can be leveraged in different cancers for different patients,” Sayour added.
CLICK HERE FOR MORE HEALTH STORIES
The study was funded in part by the National Institutes of Health and the National Cancer Institute, the Food and Drug Administration, the American Brain Tumor Association, and the Radiological Society of North America, among others.
Melissa Rudy is a senior health editor and member of the lifestyle team at News Digital. Story tips can be sent to melissa.rudy@News.com.



