Common respiratory bacteria detected in the eyes of Alzheimer’s patients
NEWNow you can listen to News articles!
A bacteria common in sinus infections and pneumonia can aggravate Alzheimer’s diseaseaccording to a recent study published in Nature Communications.
the bacteriaChlamydia pneumoniae, was found in the eyes of deceased patients with Alzheimer’s disease, according to researchers at Cedars-Sinai Health Sciences University in California.
“The retina is directly connected to the brain. It is an extension of brain development,” lead researcher Maya Koronyo-Hamaoui, PhD, professor of neurosurgery, neurology and biomedical sciences at Cedars-Sinai University of Health Sciences, told News Digital.
A COMMON HOUSEHOLD PLANT COULD BE KEY TO FIGHTING ALZHEIMER’S DISEASE
Eye-brain link
The study showed that Chlamydia pneumoniae could reach the retinal tissue that covers the behind the eye and persist for several years, creating an inflammatory response potentially related to nerve cell death. This could contribute to cognitive decline and worsen the symptoms of Alzheimer’s disease.
A bacteria common in sinus infections and pneumonia may aggravate Alzheimer’s disease, according to a recent study published in Nature Communications. (iStock)
The findings point to potential therapies for Alzheimer’s disease that would target inflammation and provide antibiotic treatment in the early stages of infection, according to Koronyo-Hamaoui.
“One hope of this study is that when people have any [symptoms of] pneumonia or atypical pneumonia or some respiratory infectiondoctors should consider performing specific tests to detect Chlamydia pneumoniae and then administering the specific antibiotic,” the researcher said.
BRAIN TRAINING SESSIONS REDUCE RISK OF DEMENTIA IN DECADES-LONG STUDY
Infection can be identified through laboratory tests, including PCR (polymerase chain reaction), blood tests, or cultures that allow living organisms to grow for analysis.
inside the studio
The researchers examined retinal tissue samples from more than 100 deceased individuals who were divided into three groups: those who had Alzheimer’s disease, those who had some cognitive deficit or those who did not have the disease.

“The retina is directly connected to the brain. It is an extension of brain development,” said the lead researcher. (iStock)
They analyzed proteins, performed genetic testing and used advanced imaging techniques on the samples. People with Alzheimer’s disease had higher levels of the bacteria in their brain and retinal tissue compared to those who had normal cognition, according to the release.
Genetic risk
Higher levels of chlamydial pneumonia were found in those carrying the APOE4 genetic variant, which is a risk factor associated with Alzheimer’s disease, Koronyo-Hamaoui added. The bacteria was also associated with more severe cognitive impairment.

People with Alzheimer’s disease had higher levels of the bacteria in their brain and retinal tissue compared to those who had normal cognition. (iStock)
The Cedars-Sinai team also analyzed human neurons and laboratory mice with Alzheimer’s disease, and found that Chlamydia pneumoniae was linked to increased inflammation, nerve cell death, and cognitive decline, further suggesting it may play a role in accelerating the disease.
CLICK HERE TO GET THE News APP
The infection also triggered the production of amyloid beta, which is a protein known to accumulate in the brains of people with Alzheimer’s, Koronyo-Hamaoui said.
While the study points to the use of the retina as a way to diagnose and monitor the disease, the researcher acknowledged that more research is needed to confirm these findings.
Experts urge caution
Dr. Aaron Glatt, chief of infectious diseases at Mount Sinai South Nassau on Long Island, New York, was not involved in the study but called the findings “interesting.”
CLICK HERE TO SUBSCRIBE TO OUR HEALTH NEWSLETTER
Glatt, who is also a spokesperson for the Infectious Diseases Society of America, emphasized that the findings only show an association and not causation, and that much more clinical research it is necessary.
“This does not mean that infections cause Alzheimer’s or that people should worry about past respiratory illnesses.”
“Chlamydia pneumoniae is a very common respiratory pathogen that many people are exposed to throughout their lives,” he told News Digital. “While the study identifies a link between this bacteria and neurodegeneration, a standard sinus infection “It doesn’t mean a patient is going to develop Alzheimer’s.”
The key takeaway, according to Glatt, is that the study opens new doors for potential diagnoses and treatments, but “is not cause for immediate alarm regarding common infections.”
TRY OUR LATEST LIFESTYLE QUIZ
Dr. Sharon Fekrat, MD, a clinical spokesperson for the American Academy of Ophthalmology and a retina specialist at Duke University School of Medicine in North Carolina, agreed that the findings could help researchers better understand how inflammation can drive disease progression and “could lead to new forms of detect or treat Alzheimer’s in the future.”
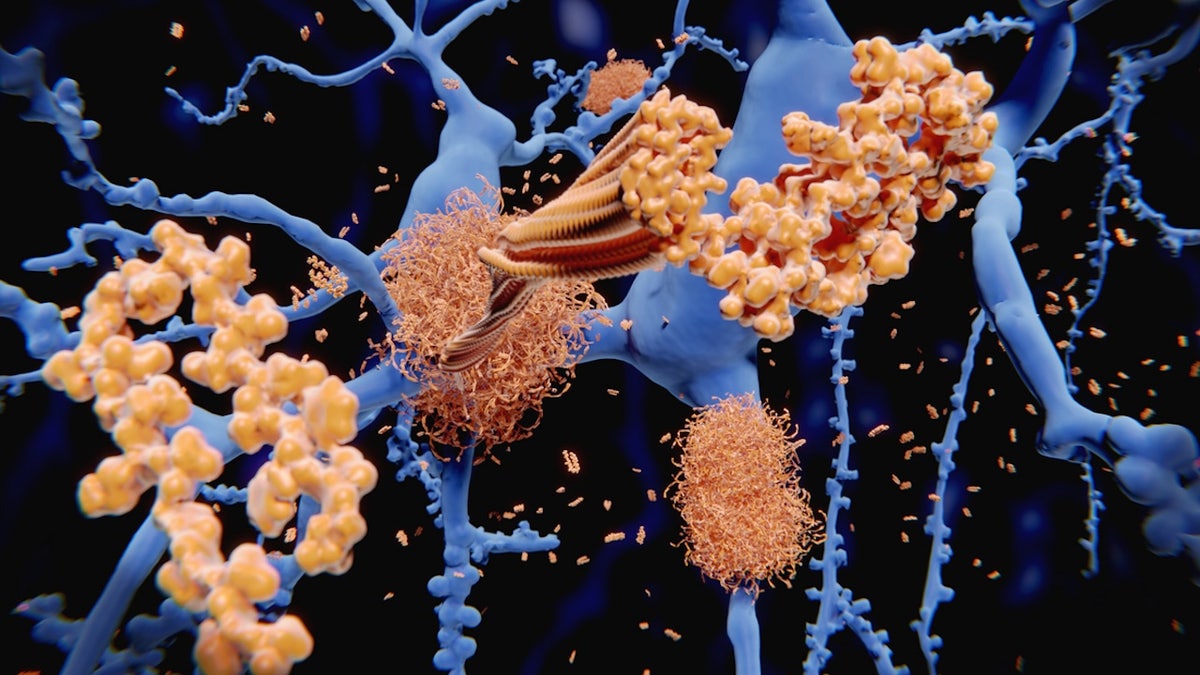
The infection also caused the production of amyloid beta, which is a protein known to accumulate in the brains of people with Alzheimer’s. (iStock)
“This is preliminary research suggesting that infection-related inflammation may worsen Alzheimer’s disease in people who are already vulnerable,” Fekrat, who also did not work on the study, told News Digital. “This does not mean that infections cause Alzheimer’s or that people should worry about past respiratory illnesses.”
What’s next?
While some teams are developing and testing retinal imaging tools in living patients, those methods are not yet part of routine clinical examinations or diagnoses, Fekrat noted.
CLICK HERE FOR MORE HEALTH STORIES
For now, the best-proven measures include following brain-healthy habits, such as monitoring cardiovascular risk factorsstay mentally and socially engaged and seek medical attention for any cognitive symptoms, the expert added.
Amy McGorry is a contributing health writer for News Digital. Follow her on Twitter @amymcgorry.



