New study questions whether annual mammograms are necessary for most women
NEWNow you can listen to News articles!
A new study suggests that annual mammograms may not be the only effective method for preventing breast cancer.
The research, published in the Journal of the American Medical Association (JAMA), tested a risk-based breast cancer screening method against standard annual mammography.
The WISDOM randomized clinical trial, led by study authors from universities and health systems across the United States, looked at more than 28,000 women ages 40 to 74, dividing them into a risk-based screening group and an annual mammography group.
ERIN ANDREWS ‘DID NOT HAVE SYMPTOMS’ BEFORE CANCER DIAGNOSIS, PURSUE FOR EARLY SCREENINGS
The researchers calculated each woman’s individual risk based on genetics (sequencing of nine breast cancer genes) and other health factors.

A new study suggests that annual mammograms may not be the only effective method for preventing breast cancer. (iStock)
Those at highest risk were recommended to alternate between a mammogram and an MRI every six months. Patients at high risk were asked to have an annual mammogram and receive counseling.
Average-risk women were recommended to have mammograms every two years, while low-risk people were recommended not to get screened until they were at higher risk or reached age 50.
A HIDDEN TYPE OF BREAST CANCER COULD BE EXPOSED BY AN INNOVATIVE NEW TECHNOLOGY
The researchers found that risk-based screening did not lead to more advanced cancer diagnoses (stage 2B or higher) compared to annual screening, indicating that it is as safe as traditional methods. However, the risk-based approach did not reduce the number of biopsies overall, as the researchers expected.
Among the risk-based group of women, those at higher risk had more screenings, biopsies, and cancers detected. Women at lower risk had fewer procedures.

The research, published in the Journal of the American Medical Association (JAMA), tested a risk-based breast cancer screening method against standard annual mammography. (iStock)
“[The] “The findings suggest that risk-based breast cancer screening is a safe alternative to annual screening for women ages 40 to 74,” the researchers noted in the research summary. “The intensity of screening was matched to individual risk, potentially reducing unnecessary imaging.”
CLICK HERE FOR MORE HEALTH STORIES
Dr. Nicole Saphier, a News medical contributor and associate professor of radiology at Memorial Sloan Kettering Cancer Center in New Jersey, said that while these findings are important, the study “completely leaves out” what screening tests are designed to do: detecting cancer early.
CLICK HERE TO SUBSCRIBE TO OUR HEALTH NEWSLETTER
“If you don’t measure stage 0, 1, or 2A cancers, you can’t know whether personalized screening tests delay diagnosis in a way that matters for survival and intensity of treatment,” Saphier, who was not involved in the study, told News Digital in an interview.
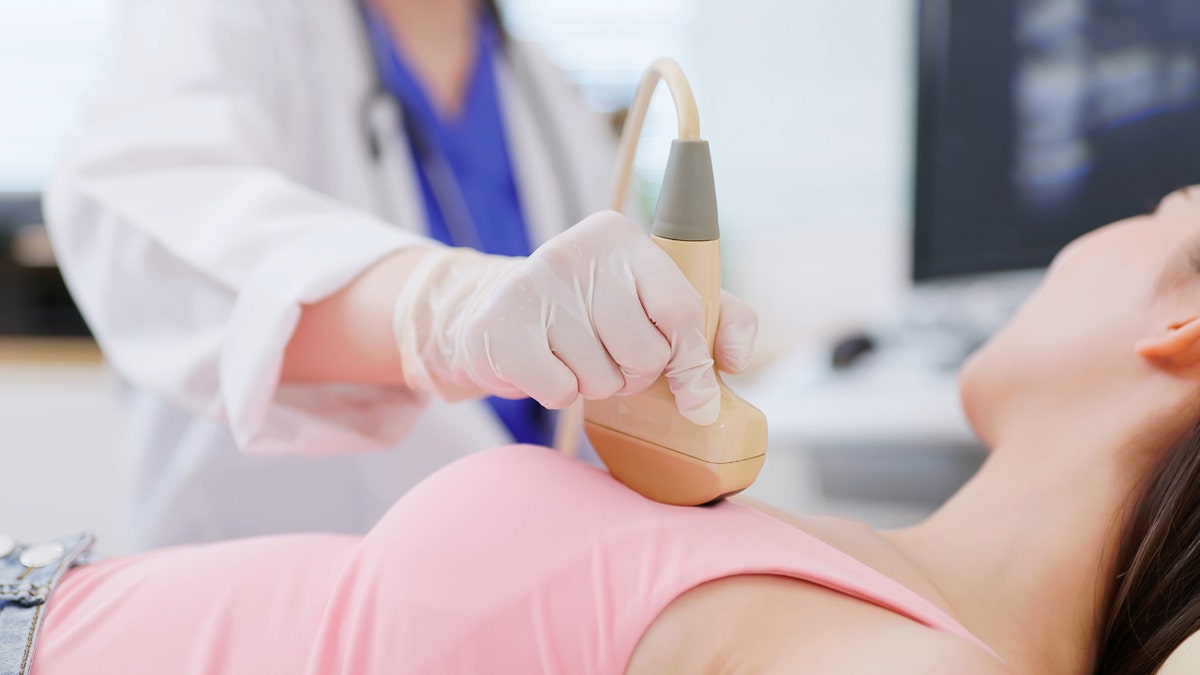
Those at highest risk were recommended to alternate between a mammogram and an MRI every six months. (iStock)
More than 60% of breast cancers in the US are diagnosed at stage 1 or 2A, where cure rates exceed 90%, the doctor noted.
The trial does not “fully evaluate” whether risk-based screening changes screening in the earliest, most treatable stages, where screening “offers its greatest benefit,” according to Saphier.
CLICK HERE TO DOWNLOAD THE News APP
“Mammography is not without risks: radiation exposure, false positives, anxiety and potential overdiagnosis are real and must be recognized,” she said. “But it remains the most effective, evidence-based tool for detecting breast cancer in its early stages, when treatment is most successful.”
The expert added that labeling women under 50 as “low risk” is “outdated,” as breast cancer diagnoses are increasing among younger women.
TRY OUR LATEST LIFESTYLE QUIZ
“Until long-term mortality data support alternative approaches, annual screening starting at age 40 for women at average risk should continue,” Saphier added. “Women’s breast cancer risk should be assessed at age 25 to determine whether screening should begin earlier.”
Angelica Stabile is a lifestyle reporter for News Digital.



